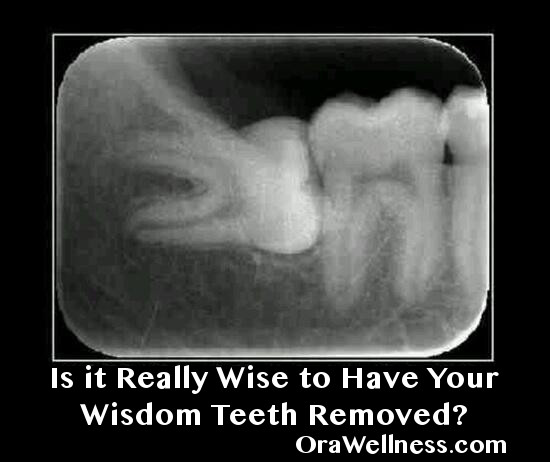
Thank you for all the recent questions around the safety and risks of having wisdom teeth removed.
In response to our recent article, titled “The Common, Unknown Risk of Having Wisdom Teeth Removed” where we share our story about a cavitation surgery, we received many questions like “Is it safe to have wisdom teeth removed?” and “What are the risks associated with having wisdom teeth removed?” among many others.
As with so many subjects in dentistry and medicine, there is no black and white/ right and wrong answer. It can be challenging to see clearly through the cultural stories around wisdom teeth removal as well as to review the scientific literature on the subject.
So, it’s in this spirit that we write to help you sort through the data to determine if having wisdom teeth removed for you or your children is the wise decision.
Wisdom teeth are routinely removed regardless of whether the tooth is infected or healthy.
But is this really necessary? Are there dangerous risks associated with this common procedure?
In order to do this subject any justice, let’s lay down a few terms so we can all be on the same page.
Impacted wisdom tooth: An impacted tooth is simply a tooth that hasn’t fully erupted into the mouth. This most commonly happens due to space limitations in the jaw. Wisdom teeth can be impacted in many different angles. Some wisdom teeth can even grow in fully sideways (strange but true).
Erupted tooth: When a tooth breaks through the surface of the gum tissue, it is erupting into the mouth. Think a child teething. Their teeth are erupting into the mouth. Wisdom teeth do the same thing and the associated slight fevers and teething pain can occur.
Dry socket: The common term for Alveolar osteitis, inflammation of the jaw bone. Dry socket most commonly occurs when the body fails to create a blood clot in the open wound after a tooth extraction. When a dry socket happens, the jaw bone is exposed to the mouth environment because the body’s ability to knit gum tissue over the gap to close the wound has been compromised. Dry sockets are very slow to heal and can be rather painful.
Paresthesia: Damage to the nerve. The mandibular nerve is very close to the roots on lower wisdom teeth. Removing impacted lower wisdom teeth can unfortunately cause permanent damage to the nerve resulting in frequent drooling, loss of sensation on the lip (which can cause frequent biting of the cheek) and diminished ability to taste (and enjoyment of kissing 🙁 )
With these in place, let’s take a closer look at the main cultural stories we have around wisdom teeth.
Myth 1: Wisdom teeth have a greater tendency to become diseased.
It makes sense that the dental profession would come to this conclusion. After all, they are seeing a portion of the public who make appointments with them to get their help with stressed teeth.
However, the stats say that only 12% of impacted wisdom teeth become diseased. While 12% may seem high, if we consider that 10% of appendix become diseased and we as a culture don’t remove healthy appendix just to avoid the risk of the 10% that become diseased, why should we remove healthy wisdom teeth? Clearly, not because there a huge risk of the wisdom teeth becoming infected.
Myth 2: It’s easier on the body to take wisdom teeth out earlier in life.
I can understand the rationale behind this myth. After all, it makes sense that an 18 year old would bounce back easier and faster than a 48 year old to having some surgeries in the mouth. And in a way, we agree with this given the 18 year old’s immune system has, in theory, had to deal with less stress so may have an easier time bouncing back.
However, again the research falls short of backing up this myth. In fact, risks of secondary infection, paresthesia and developing a dry socket are higher among patients aged 12 to 24 than patients 35 to 83 years old. The highest risk of secondary problems from having wisdom teeth removed lies in the age group from 25 to 34 years old. (1)
Myth 3: Leaving wisdom teeth intact will cause your teeth to shift and get misaligned
We find that this ‘reason’ is the most common myth about leaving wisdom teeth in the mouth. In fact, a quick scan on the net for reasons to have wisdom teeth removed found an article on WebMD which states crowding other teeth as the #1 reason to have wisdom teeth removed. “Damage to other teeth: That extra set of molars can push your other teeth around, causing mouth pain and bite problems.” (3)
Again, research trumps cultural myth…
To quote Dr Jay Friedman, “Third molars do not possess sufficient force to move other teeth. They cannot cause crowding and overlapping of the incisors”. (2)
To add to this, other studies have been conducted to determine whether wisdom teeth really can cause our teeth to become crooked. Authors state, “There are valid reasons for extracting third molars. But extraction for the exclusive purpose of relieving interdental pressure and thereby preventing incisor crowding is unwarranted.” (4)
Myth 4: You increase the risk of disease if you wait to have them removed.
They are way back there in the mouth. You can’t clean them as easily. Of course they are going to become infected and be a breeding ground for disease throughout the mouth, right? 🙂
“There is no evidence of a significant increase in third-molar pathology with age.” (5)
That sums it up I think…
Myth 5: There’s little risk removing them.
Little risk? This article is dedicated to a recent sad statistic of a 17 year old young woman who is nearly dead after going into cardiac arrest toward the end of having her wisdom teeth removed.
Unfortunately, the above recent event isn’t unique. Here’s a story about another 17 year old young woman who died from this ‘not risky’ procedure.
Less ‘serious’ risks of having wisdom teeth removed range from dry socket, damage to the jaw joint, and jaw fractures to permanent paresthesia. In fact, in some types of impacted wisdom teeth (namely when the wisdom tooth is tilted toward the second molar), the risk of nerve damage is as high as 6%.
Now, 6% may not seem like a very high number, but would you risk drooling for the rest of your life due to nerve damage if you actually knew the statistics? I know I wouldn’t put any children in my care at risk of this unless I was given a very good reason (backed by science not myth).
Dr Friedman puts it rather matter of factly, “There can be no excuse for tolerating so many unnecessary extractions on millions of unsuspecting and misled people and putting them at risk of so much iatrogenic [dentist induced] nerve injury. This is a public health hazard.”[emphasis mine] (2)
So when is it a wise consideration to have them out?
If the tooth/teeth give you regular challenge, then the benefit to have it/them removed may outweigh the risks. However, what we hope this article has helped you realize is the folly to have healthy wisdom teeth removed to ‘save us’ from the damage that invariably will happen.
This notion simply isn’t based in reality. If your dentist tries to pitch these unsubstantiated claims as reasons to have wisdom teeth removed, vote with your dollars and find another dentist who is willing to work with you and stick to the science.
Let’s wrap this subject up with a couple quotes. “The fact is that most third molars, impacted or not, do not become diseased and that the risk of iatrogenic injury [dentist induced injury] from such surgery is greater than the risk of leaving asymptomatic, nonpathologic teeth alone” [emphasis mine] Jay Friedman, DDS, MPH”
Bottom line, if the tooth isn’t bothering you, best to leave it alone. To quote our long time mentor and friend, Dr David Kennedy, “God gave us 32 teeth for a reason”. Maybe we shouldn’t mess with that unless really necessary?
What about you? Do you still have your wisdom teeth? If so, have they given you any trouble? Did you have yours out? Has that given you any trouble?
Helpful, related resources:
The Unknown, Common Risk with Having Wisdom Teeth Removed
References:
1. Osborn TP, Frederickson G, Small IA, Torgerson TS. A prospective study of complications related to mandibular third molar surgery. J Oral Maxillofac Surg. 1985;43:767–769.
2. Friedman J. The Prophylactic Extraction of Third Molars: A Public Health Hazard. Am J Public Health. 2007 September; 97(9): 1554–1559.
3. http://www.webmd.com/oral-health/guide/wisdom-teeth-removal-necessary
4. Southard TE. Third molars and incisor crowding: when removal is unwarranted. J Am Dent Assoc. 1992;123: 75–79
5. Stanley HR, Alattar M, Collett WK, Stringfellow HR, Spiegel EH. Pathological sequelae of “neglected” impacted third molars. J Oral Pathol. 1988;17:113–117.

My girlfriend has a situation somewhat similar to the x-ray at the top of this article. One of her wisdom teeth is growing in sideway or at more of a diagonal angle.
The dentist we saw recently said she should remove this tooth especially as it is causing issues for the molar it is pushing against horizontally. There is also a gap between the junction of these two teeth that may trap food particles and lead to other issues.
Has anyone else also experienced this issues? Any insights to offer or recommendations for second opinion?
We have the x-ray images and would be easy to share online.
Aloha Nathan,
Thank you for your comment!
We’re sorry that your girlfriend’s wisdom tooth is growing in sideways or at a diagonal angle.
We here at OraWellness aren’t medical or dental professionals, so we can’t treat, diagnose, advise, etc. Instead, what we can do is share information with you to help you become self-empowered on your journey.
A good dentist can be hard to find, but once you find one, they can really be a dream for helping us play detective to figure out what might be going on and answering more questions on stuff like this. Remember that they are here to serve you, and you can choose who you are willing to work with. And in situations where we feel uncertain about a diagnosis that’s been made or a procedure or treatment that’s been recommended to us, it can be helpful to get a second professional opinion.
Here’s an article that explains how to find a dentist: Helpful Resources to Find a Qualified Dentist to Assist You
Also, here’s a helpful tip: if you find a holistic practitioner (doctor, chiropractor, nutritionist, etc.) that you like and respect, you can always ask them who their dentist is or if they know of any dentists that they approve of in your area.
Finally, it can also be helpful to Google reviews on the different holistic practitioners, dentists, and organizations that you encounter so you can see what kinds of experiences other folks have had with them.
I hope that helps!
Aloha! 🙂
Thanks for the info! I normally agree with you all on these articles, but in my case, I did wait 10 years to have my wisdom teeth removed because I was concerned about the health risks. Waiting 10 years caused me to be in pain for too long to the point where I needed to have them removed ASAP. It did make it harder to clean that area because they were impacted. I was in a lot of pain, and I definitely needed to have them removed. My mouth was could not contain them as there was not enough space. It was wise to have them removed, and I think the body is wise: I don’t think there would have been pain unless it was necessary for me remove them, and yes, they told me it was causing all kinds of issues. I went with a skilled surgeon, and the area healed well. I don’t regret removing them. I felt relief after I healed, and I never was suffering from the pressure they were giving me. I’m glad I waited, but I think in certain cases, it is important to remove the wisdom teeth for people who don’t have enough space for them. As for the majority of people who don’t have pain, but who are told to remove their wisdom teeth for precautionary reasons, I think that’s not wise, and the decision should be done with precaution. But I had a good experience with the surgery because I had a skilled surgeon. I think it’s a big deal to remove one’s wisdom teeth, and the decision should be heavily researched, and the pros and cons should be considered. I waited 10 years deciding the pros and cons, and in the end, removing them was the wisest thing for me.
Thank you so much for this information.
I had my wisdom teeth extracted when I was 15 years old… they weren’t completely formed at the time and they were coming in underneath my second molars.
One day I started having intense pain on my lower left jaw where my second bottom molar was being sandwiched between the wisdom tooth coming in underneath it and the molar on top when I would bite down.
I ended up forming an abscess there on the gum next to the second molar, I was told I had an infection on my jaw bone, and the hope was that removing the wisdom teeth would resolve the issue. I’m guessing this would be a situation where removing the wisdom teeth might be a good idea.
The doctors decided to remove all four wisdom teeth at the same time since they all similarly looked positioned to come in under the 2nd molars.
We pulled them. I continued to have the abscess and pain in the second molar, which turned out had died, maybe from damage to its root, and a year later that one was pulled too.
I am 36 now and have continued to have discomfort and pain in the area of my mouth ever since. The scar from the abscess is still there but hasn’t been open ever since the second molar was removed and healed.
I started seeing a Holistic Dentist a few years ago with the specific hopes of checking for a cavitation. She simply looked at my xrays and in my mouth and determined there was no cavitation. I will look into some thermal imaging as you have suggested… I live in San Diego so lucky me, I can check with Pink Image. I am curious what kinds of immune supporting protocols you might recommend in leu of a cavitation surgery if it turns out there is still an infection there however I’d be open to a surgery if that would be helpful too.
You guys are absolutely amazing… I am so grateful for the thorough, conscious, caring effort you put it to helping educate and empower us. <3 You've just helped uplift me in my health and wellness journey to a whole new level. Thank you, thank you!
Aloha Alexandra,
We’re sorry to hear about your ongoing dental difficulties!
We here at OraWellness aren’t medical or dental professionals, so we can’t treat, diagnose, advise, etc. Instead, what we can do is share information with you to help you become self-empowered on your journey. Now that we’ve got that out of the way, let’s see what information we can share to help. 🙂
We share some system-wide immune support strategies in our recent article titled, “Is It Possible to Stop a Dental Abscess?”.
Also, in case you’d like to check it out, this article shares some info on cavitations: “The Common, Unknown Risk of Having Wisdom Teeth Removed”.
Thank you so much for your kind words of support! We’re honored to play a role supporting you on your journey to optimal oral (and whole body) health, Alexandra. 🙂
My brother says that he has teething pain and he can stand it sometimes. I like how you mentioned that erupted tooth can provoke that feeling. I will help him look for a dentist that can do him a wisdom teeth removal in case he needs to.
Do not ever go to a dentist for wisdom teeth removal. You must go to an Oral surgeon who has far more education on removing wisdom teeth and also more knowledge in the placement of the needle so as not to hit the nerve. Oral surgeons are never taught to pull the tooth they are taught to elevate the tooth therefore causing less trauma to the mouth find yourself a good oral maxi facial surgeon. One that is concerned about you and the problem and not his wallet. My husband was an oral surgeon for 50 years but unfortunately he passed away seven years ago at the age of 74 he loved what he did and he never got rich doing it because he loved his patients
My dentist advises to remove my upper wisdom teeth, as because my lower ones have been removed a long time ago, my upper wisdom teeth are now starting to drop down. There is already a bit of dentine visible and my dentist says that at some point it will be impossible to clean between the wisdom teeth and neighbor. And also that it will start to bump against the lower molars. What’s your opinion?
Coming from England & In my mid 40’s I still have all of my 4 wisdom teeth intact & they’re straight too. Never had a single problem with them. U.K. Dentists only remove if there’s a valid reason to. My first lower 3rd molar came in at age 23 they tend to be slow growing in & can take several years until they become a fully mature tooth, well that’s been my experience anyway. My second lower wisdom the other side erupted at age 36 & is still growing, about 2/3 of the way in now & healthy. My dentist in North America has said he won’t remove my top wisdoms which haven’t erupted yet, although other dentists say they’re impacted & recommends they be removed. I believe my Dad didn’t have a wisdom tooth come through until he was in his 60’s. Well they do call them wisdom teeth for a reason.
Such a great article. Thanks a lot for sharing this. I am 41 year old female. I had my 4 wisdom teeth erupted in my 30s. The process was painful for one upper jaw tooth as there was no room for it to erupt. But it came out fully. I was in pain for some days. Or Weeks. But I realized that the tooth was broken from top and while checking a bit of it came off easily.
Now there is only root. But no pain. Other 3 wisdom teeth are healthy.
What should I do with the root remaining. I feel no pain. And I really don’t want to get it removed.
Kindly suggest.
Thanks.
Will appreciate your reply.
I am 21 and I am getting my wisdom teeth at this point,in my lower jaw. I’m in much pain as I am not able to open my mouth or chew properly. It has been 3 days since I am suffering from this. I wish the pain ends soon because it’s very painful.
Interesting thoughts about removal of wisdom teeth. My 19-years old twin-daughters have just had all their wisdom teeth extracted because of small cavities. My daughters have great teeth with only few fillings (3 and 5) but dentist said the wisdom teeth would most probably have more cavities later and therefore fillings in wisdom teeth were waste of money. When I was about their age I also had cavities in my perfectly erupted wisdom teeth. At that time I had them drilled and filled with silver fillings and recently I had these old silver fillings replaced by new white fillings. I have lived very fine with fillings in my wisdom teeth and I guess my daughters could do as well – maybe things have changed when it comes to dentist’ view on decayed wisdom teeth?
I really like what you had to say about wisdom teeth and why it can be important to have them removed for reasons like impacted teeth. This is something that I am worried that I have because my teeth are really hurting in the back. Maybe I should go to a dentist and get a professional opinion on my wisdom teeth and if I need them to be removed or not.
Just a quick testimonial for keeping wisdom teeth . . . I ignored my dentist’s advice to remove my impacted wisdom teeth at age 22 just because I had better things to do and they didn’t bother me. Fast forward to now (age 49) and I still have them all. The only time one bothered me was at age 34 – after I started to drink raw dairy for a couple of months one of them straightened out and emerged as a brand new tooth! I went through some teething pains but it was worth it!
It’s funny – my current dentist was measuring my gum pockets (I had moderate periodontal disease which has since gone away from using your HealThy mouth formula) and he didn’t know what to call the space between the impacted wisdom tooth and the back molar – as if he’s never seen that situation before (someone my age with with “intact” impacted wisdom teeth). Just goes to show you how routine wisdom tooth removal is.
I was told at age 17, and again in my 20’s, that I have no wisdom teeth. However, I found out at age 35 that I do have one on the upper right side, fully impacted. The dentist said that we could just keep an eye on it, and if it didn’t cause any problems down the line, then I could probably live my whole life without doing anything about it. He said that the only real difference is, prior to my appointment, I didn’t know it was there, and now I do. His only concern was that, if it does need to be removed for some reason when I’m much older, say in my 70’s, then it could be harder for my body to handle the surgery. I’m 44 now, and my approach has been to just live my life as if it’s not there, because I haven’t noticed any negative effects of it being there. I wouldn’t dream of having it removed just to have it removed. Thank you Will and Susan, for all that you do!
Thanks, this article confirms my decision to leave my four wisdom teeth in my mouth 🙂 My dentist almost convinced me to have them removed and I even went to an oral surgeon for an initial consultation, but after doing some research, I concluded that it wasn’t worth the risk – especially since they weren’t bothering me! They used the “it’s hard to clean back there so eventually they’ll rot out of your head” line, but now years later the hygeniest comments on what a geeat job I do keeping them clean!
We do Craniosacral Fascial Therapy and find most people have issues with the fascia in their mouth due to extractions, injections, etc. Everything we do to our bodies has an effect. And often the effects of things done to our mouth are seen in other parts of the body.
The last give me so much pain one time. After some time I go to the doctor and he cut it off from a side. Is there any problem that I need to face in future?
Our dentist is telling us our 17yr old daughter has to have her wisdom teeth out. Reason for the top is you can see them already growing into the root of the second molars. Reason for the bottom if she has to get them out later it raises her chance of nerve damage.
I hear you saying with an angled bottom the risk to the nerve is during extraction. Why does my dentist site this as a reason for extraction?
Ps my husband and I both still have all our wisdom teeth despite being told many different reasons to have them out. Not enough jaw bone, impacted etc.
I just pulled out my bottom two wisdom teeth. No issues except for the annoying holes which are now there where the teeth were. Food gets stuck. When do they usually close up?
Also my dentist is suggesting to remove the top two wisdom teeth too, but they are straight and perfectly fine. Do i need to go through with it?
Wow. I didn’t know the statistic for nerve damage relate to wisdom tooth removal is higher than 5%. I usually ask and listen to recommendation from my dentist. I had two of my right wisdom tooth removed because they were both bothering me. The upper right was at an angle that always cause sores, while the lower right is tender and was recommended to be removed by my dentist.
Now I am experiencing with pericoronitis on my lower left, while my upper left is fully impact inside the jaw. I am in so much pain when I am swallowing. I can feel the pain all the way down to my left side of the throat. It is annoying trying to sleep because my wisdom tooth hurts, and the extra saliva production create the need to swallow. It is super annoying and painful. I visited a new dentist and was recommended to have it extracted, with an offer to have it done that same day. The new dentist said the wisdom tooth is far enough from the nerve to not cause any damage, but I am hesitant. Last fall, when I visited my usual dental provider, I was told the lower right was closed to the nerve. They had to consult an oral surgeon or someone I believe have more knowledge about tooth extraction. But he only comes once a month. He did say it was possible, under general sedation. He did not want me to move because of pain. I am glad that they are taking precaution. The new dentist appeared to offer a removal with local anesthesia as the cost was 400. Maybe the tooth moves up enough that it can be removed with less chance of damaging the nerve.
I was suggested to wash my mouth with salt water to help with the pain and swelling. No antibiotic was prescribed, but I am dealing with chills that indicate a slight fever. I am taking ibuprofen to help with the fever and it appears to be doing great. But, the fever comes back once the pill starts to wear off. I am just trying to clean that area with brushing, wash mouthing with hydrogen peroxide, then baking soda to fight off this painful issue. I will soon be visiting my usual provider a day after for a second opinion.
I was also recommended to have the upper left wisdom remove even though it was not problematic for me. The usual provider said, this wisdom tooth may never pull through out of the gum. But it is in an awkward position where a portion of it top the teeth beside it. I am just worry that if it starts pushing out, I could feel a lot of pain. But it seems this wisdom tooth is very far up. I am worry that removing this may cause some kind of opening into my sinus which is why my new dentist recommended I go to an oral surgeon. They will be equipped to close it if required, the staff explained to me.
I just saw my dentist and he wants to remove all four of mine, even the 3 that are healthy in order to prevent possible problems in the future. I’m unsure what to do now after reading this article. I will say this though: the myth about them not having the ability to move other teeth is NOT a myth. When my bottom ones came in they messed up all my bottom teeth, causing ones near the front to go from perfectly straight to very crooked, and causing a molar and one other tooth to be pushed inward toward my tongue. Experience always speaks louder than opinion, even an educated opinion.
I have the exactly same issue on my lower jaw. Had nice and straight teeth and ever since my wisdom teeth started growing, it started pushing the other teeth. Now my first incisor is completely out of line and both fifth teeth are turned inwards. The dentist suggests removing the wisdom teeth but I was always terribly scared of tooth extractions (thankfully I never needed any so far) and now I know why. Is it possible that my teeth will become straight again once the wisdom teeth are removed?
I am seventeen years old and I still need braces for teeth that are crammed in the front as well as an overbite. I have not been able to get braces yet because my sisters’ teeth needed braces asap and my mother couldnt pay for all three of us at once. Now it is my turn to get braces which will help with a lot of the problems I have with my mouth. Since I will be going to college soon, my dentist recommended that I get all four of my impacted wisdom teeth removed and gave me a refferal. They wouldnt tell me if or why it was nessecary and gave to my mother. Now my mother wants me to get my wisdom teeth removed as soon as possible, but I want to get the braces I have been waiting for five years four. I try telling her that my wisdom teeth have never caused me any problems that I could tell, and my overbite has caused many problems. I would rather have braces than have my wisdom teeth removed but it feels like no one will listen or talk to me because I am a minor.
Hi would like to ask if do i have to agree with my dentist? My my 1st molar are already gone and now im scheduled for the removal of my 2nd molar (leftside down part) but my 3rd molar is completely fine and healthy but the dentist suggested me to remove it as well.. should i have to agree with her or just let my wisdom tooth stay? Thank you…
Aloha Jhing,
Thank you for reaching out to us with such a truly precious question. This question is so important and is unfortunately a very rare question we ever ask ourselves.
Our answer is no, you do not have to agree with your dentist. In fact, we consider it important to not assume any suggestion/advice as true without putting it up against your intuition and reason. That’s why our ‘song’ is so well spoken from a dear friend (and AMAZING musical artist) India Arie, “Stand up for your rights. Keep shining your Light. Show the world your SMILE!”
Ask your dentist for proof that their suggestions are logical. If there is nothing wrong with a tooth, why would anyone reasonable suggest removing it?!?
We hope this helps you.
This article was very helpful to me! I am in the middle of a dental journey with my 21 yr old daughter… we went to a dentist who left some decay under a filling (per my bio dentist eval) and she had to have it extracted…she was 5 yrs out from braces and we really didn’t think much about it, til she told me her teeth were moving…we then went to our new dentist who said that besides the gap of extracted tooth, she has another tooth next to it that is moving and has left a big gap…so, off to the orthodontist to get her upper retainer back in and he says that he can’t do that now, as it has shifted too much and will need the wisdom tooth removed, so he can put a small bracket/braces area to move that tooth or my other dentist won’t be able to get the implant in, which the lack of, has already caused my daughter’s jaw to pop loudly and often…the chiro helped with it, but said that it won’t get better until she can eat on the side with the gaps more equally. Help! I don’t want to take a chance on any lifelong issue for my daughter… one dentist is saying that without an implant/partial, my daughter has a lack of integrity in her jaw and now, I am understanding that removing a wisdom tooth can also cause that lack of integrity…I am speaking with 4 different dental professionals and none are on the same page…I really could use an unbiased opinion to help us make the decision… I am thinking of asking if they can just remove any of the gum flap tissue and leave the tooth… what do you think? Love your site and I post it regularly on my FB group! (: Blessings! Evelyn
My wisdom teeth has been delaying to come up for years am 26 now my gum at that point that it has been trying to come up is always paining me was should I do
idea: that wisdom teeth removal is a revenue driver of the dentistry sector, and that they often recommend it unecessarily
I was told I needed to get my wisdom teeth out (though not immediately) because they are growing out sideways toward me cheek. I don’t experience pain but I do not have full range of motion in my jaw because of it in some positions. Honestly they don’t bother me but I am concerned that I should get another opinion as to the urgency now that it is years later. I am looking for a dentist who agrees with the body healing itself rather than surgery- can you recommended a network where I can search for a dentist in my city in Austin Texas?
Aloha Dana, Thanks for reaching out to us here!
We’re sorry your wisdom teeth are growing out sideways.
Here are helpful resources to find a qualified dentist to assist you
Hope that helps!
Great advice for those who are considering having their wisdom teeth removed. It’s important to understand all of the risks on both sides of the argument. Thanks so much for sharing.
I’m really surprised that third molars don’t have enough pressure to move other teeth. I always thought that my crooked canines were from my wisdom teeth being removed too late in life. I eventually got braces to fix my smile, but I always blamed my wisdom teeth.
Do you know if there is any information available on how long the erupting process is? I tried google and I couldn’t find any!I have one wisdom tooth that started erupting about 4 months ago and it’s still only partially through the gum, so I’m trying to find if that’s normal or not. I’m also wondering if I only have the one, or if the others just don’t have any room to come in. If I only have the one, would I still be able to keep it if it doesn’t have another tooth to press on? It’s coming in pretty straight, and it’s a bottom tooth if that makes any difference.
Aloha JT,
Thanks for stopping by and asking us.
Wisdom teeth definitely can take their time coming in. Sometimes they stay partially erupted (which can present its own complications). One thing you can do to help it come in is to put the tooth to use by intentionally chewing on something. Think of when a young child is teething. We naturally want to give the child something tough to chew on since the chewing is going to help the tooth fully erupt into the mouth.
At the risk of concerning you, leaving a wisdom partially erupted isn’t wise as the tooth is going to be more prone to decay and the gum around a partially erupted tooth is a great hangout for the ‘bad bugs’ implicated with gum disease.
We hope this helps you!
I sort of remember when I got my wisdom teeth removed. I was 18 at the time and I think if I didn’t get them out, I would be facing more dental pain and issues today. Sometimes, it might be better to leave it alone if it isn’t giving you any problems. Then again, it could give you problems in your later years. For whatever opinion you have, I’d first want to talk to a dentist and see what they have to say. Let their experience do the talking and see if surgery is right for you.
Thanks for sharing these myths and truths about wisdom teeth and their impact on your overall dental health. I think it is so awesome that only about 12% of wisdom teeth become diseased. Although that is a higher number than for other teeth, it is nice knowing your teeth won’t automatically become diseased just because you didn’t have them removed. However, I think that it is also important to not discount that impacted wisdom teeth could end up being a problem, especially if you don’t catch it early enough.
Aloha Delores,
Thank you for stopping by to offer your input.
We completely agree with you that it’s important to not discount the fact that wisdom teeth, especially those that are only partially erupted into the mouth, can be a wonderful ‘safe haven’ for bad bugs in the mouth. The fact still remains that unless our oral hygiene pays particular attention to any areas of challenge in the mouth, we’re asking for trouble. Wisdom teeth are more challenging to keep clean as they are ‘way back there’. This is true particularly for people with small mouths or those who have jaw issues so can’t open as widely as necessary to really be able to clean properly ‘back there’.
Thanks again for sharing here!
Hi there, im 29 and both of my lower wisdom teeth are somewhat sideways with a slight angle upwards, not quite as extreme sideways as the picture above.
they are creating some very deep pockets ( about 9-10mm) when i water pick them alot of bad taste comes out from all the bacteria brewing back there. the dentist recommends i have them removed.
i find if i waterpick frequently that the gums around them look better but i feel that overall it always lets bacteria grow and causes bad breath.
what would you do?
Aloha Sean,
Thank you for reaching out to us. Your story sounds very, very familiar to us (from personal history about 20 years ago now).
The name of the game is to keep the area clean, ‘disrupt and disorganize’ the bad bugs and allow the regrowth of the good bugs to colonize in those gum pockets. You can do this several ways.
Removing the teeth will accomplish this as you won’t have the deep pockets any longer. An oral irrigator device can help, but they are difficult to get to the bottom of 9-10mm pockets to clean AT THE BASE of the pocket which is the super critical place needed to disrupt and disorganize the bad bugs.
At the risk of sounding like I’m trying to sell you something, we literally created our Healthy Mouth System for exactly your situation. You see, it’s tricky to be able to keep the area clean and consistently disrupt and disorganize the bad bugs implicated with gum disease (that’s the smell you reference) without the proper tools and education.
Whatever route you choose, use the smell as your guide. You know how infection smells now so you can always use that to track your progress. Susan got so sensitized to the smell of gum disease that we both now can smell if a person has a bad infection if we are in the same room with them.
We hope this helps you along your path Sean. Thank you again for seeking solutions here with us. We are honored to be part of your path.
I have been stunned by the dramatic improvement in gum pocket depths in my own mouth over a year of rather casual, even sporatic following of the Heal Thy Mouth system. Four sequential professional oral exams have documented 1-3 mm of improvement in dozens of my gum pockets, as well as regrowth of gum recission.
So simple with the tools and instructions I obtained here. All for less than the cost of one serious filling.
Hello, my 18 year old son has a wisdom tooth that looks like the picture above. Its growing sideways. Any recommendations?
Thank you,
Yoli
Aloha Yoli,
Thank you for stopping by. We are honored you chose to ask us for our opinions here. Of course, we can’t make any suggestions or offer any course of treatment. What we like to do in situations like this is ask ourselves, ‘what would we do?’ and share that. Please find a dentist who has a ‘helper’s heart’ and knows their stuff to help guide this for your son.
Depending on whether it’s an upper or lower wisdom tooth, I would most likely just leave it as is (presuming it’s not causing any problems). The research for complications and potentially permanent nerve damage from removal is most common with wisdom teeth (particularly lower teeth) that are coming in at an angle similar to this. So, please be very careful if you hear, “We take these out all the time with no problem” because the research does not support broad (potentially arrogant) statements like this.
I hope this helps you navigate this path with your son. If the teeth bother him, they may need to be dealt with. That doesn’t mean they have to be surgically removed however.
Thanks so much Will. His sideways wisdom tooth s on the bottom.
I’m one of the lucky ones that have 32 teeth! My wisdom teeth started to erupt when I was 13 years old. It was painful of course, I remember rubbing a topical analgesic on them to numb the pain. I’m so glad that my parents didn’t run me to the dentist to have them extracted. 47 years later they are still in my head and disease free! I even have a crown on one of them…I’ve always thought it important to keep all my teeth! As far as dental hygiene goes….all 32 get brushed and flossed several times a day, it’s not any harder to take care of 4 more teeth!,,
Aloha Lauren!
Thank you for stopping by to share your story with us! Congratulations on having parents that didn’t buy into the cultural stance on wisdom teeth! Good on you! 🙂
Since I didn’t know any better, I had my two wisdom teeth on top removed but it was more so because I was having jaw surgery the following summer and the surgeon wanted to remove the wisdom teeth prior to the surgery. Is there a reason why some people only have wisdom teeth on the top and not on the bottom and vice versa? I have always been curious why I didn’t get wisdom teeth on the bottom. I wish I didn’t have to go through jaw surgery but I was a thumb sucker and my front top teeth didn’t even touch my front bottom teeth – just a gap/hole that made it quite easy to squirt water through when I was younger 🙂 One other question not related to wisdom teeth – why do people sometimes have missing adult teeth? My father had a missing adult tooth and then I must have inherited that trait because I also had a missing adult tooth under one of my “baby” molars. Thank you very much for your time! I love your products!
Aloha Alexis,
Thank you for reaching out to us.
We don’t know why it seems that some people don’t develop all 32 teeth. It seems to me as kind of a human experience of the work of Dr Francis Pottenger. Dr Pottenger did some fascinating research with cats and nutrition. What he found is as a species is nutritionally deficient over generations, the genetics stop fully expressing with what is a ‘complete’ animal. I’m getting ready to write an article titled something like “What generation of Pottenger’s cats are you?” that will discuss this in more detail.
I think each of us can look at our family history and see how far back we have to look until we find a generation that ate what the human body really requires to optimally thrive. I know in my own family line, I can’t see far enough back to see any quality nutrition! 🙂
The good news of Dr Pottenger’s work is once he started feeding the malnourished cats better, their genetic expression improved dramatically! So, the moral of the story is to make positive changes today knowing full well that our health (even genetic health) improves immediately.
Thanks for giving us the platform for sharing this idea with you!
As always, we appreciate you stopping by to share with us!
Aloha!
My own guiding principle is always to try anything that offers to stimulate natural health while keeping all my body parts intact before “trying” surgery.
I would put wisdom teeth pretty low on the list of possible causes for headaches and insomnia. Possible, but not probable.
Sugar is certainly higher up on the list of causative agents for caries and headaches. Many parents can testify that it can also be a dramatic cause of failure to fall asleep.
Chiropractic has a wonderful record of resolving the cause of chronic headaches (both tension and migraine types).
Will and Susan recently published an article that could probably be read under the title of “4 Simple Ways To Help Resolve Chronic Headaches and Improve Sleep for Your Children and Yourself.”
I meant my left eye twitched for a month after..
I am 44 with all my wisdom teeth either chipped or broken due to cavities. They do cause pain when I don’t pay attention to my diet. Food gets lodged in the cavities & I usually do Water Pik to keep them free of any bits & pieces. Recently though my wisdom teeth ache when I just press on them. However, I can manage the pain when I take BioDent tablets (10/day) & a Tbs of FCLO regularly. I had one of my Mercury fillings replaced a few years ago on my bottom righ side & for one month after, my left twitched consistently as a reaction. These things really freak me out as I don’t know how my body will react to an actual extraction. I would love to figure out if there is any way remineralize these teeth so that I don’t have to extract my wisdom teeth..but am not sure that it is possible with the condition they are in..
I had my top wisdom teeth removed, sever crowding, and no issues with the removal when I was 14. My bottom never came in and really do jot give me trouble. I think they are pushing on the other molars though. They have started to come through the gum. I am debating on weather to remove them or not. Looking for a dentist I can work with. Thank you for the article.
I say listen to your dentist & what he says & make sure he shows u the x rays too, I had 3 wisdom teeth out as a sml mouth & no room, they properly thru too, I believed him as I could see what he meant as I def had NO room, however I have 1 left causing no problems & 2 dentists gave the same opinion that let sleeping dogs lie, if its causing no problem l say what works for u & your dentist,
I am no professional and can only share that as a20 yr old, my teeth began to turn, had always been straight, had my wisdom teeth, the three I had, removed with no complication and my teeth did straighten out. This may not be true for everyone, but it was for me. That said, I do not plan to have my children’s removed unless there is an issue.
Aloha Shannon,
Thank you for stopping by and sharing your experience with us. I’m curious if your wisdom teeth were upper or lower that you had removed (you mention 3). The research shows that lower wisdom teeth don’t cause the teeth to shift, but I didn’t find any info on upper wisdom teeth. I hope that our article simply helps to open our cultural eyes to the fact that just because something is common doesn’t mean it’s normal. It’s worthy of taking a close look at the habitual removal of healthy wisdom teeth.
Thanks again!
Hi. When I was around seven years old, a dentist measured my teeth and mouth and reported to my mother that my teeth were too big for my mouth. He recommended extracting four bicuspids (one in each quadrant) so that my third molars would have room to erupt when they came in. My mother would hear nothing about removing my permanent teeth and left the office without seeking another opinion. When I was eleven my teeth had come in all crooked. Another dentist removed the four bicuspids, and I had to wear braces for two years and a retainer for two years. But when my wisdom teeth came in, they came in perfectly and without incident. My teeth are now straight, and I don’t have enough room for another tooth. I have been asked by a dentist (who asked solely out of curiosity) if I would not prefer to have the wisdom teeth extracted, and I told him that the teeth are doing fine, I have gone through too much trouble to keep these teeth, and I am not about to have them pulled. I even had him put a gold foil on the number one tooth.
Aloha Eileen,
Thank you for sharing your story with us! Good on your mom for having the courage to walk out of the dental office. We need more moms like yours these days! 🙂
I had my lower wisdom teeth out 2 years ago. The left extraction site took a long time to heal and caused me a lot of pain. Later on in the year, I kept getting headaches and finally pinpointed the pain to be coming from my jaw. Since my mom and sister both have TMJ issues, I immediately made an appointment with my dentist. He said that I was definitely grinding my teeth and after discussing it with him, realized that I started clenching my jaw when I got stressed. I asked him why it just started happening now, and he mentioned my wisdom teeth extraction. I told him that the left side was absolutely awful and that the surgeon admitted having difficulty with that side. My dentist believes that a ligament (or something?) may have been damaged while the surgeon was getting my tooth out which somehow made me more susceptible to clenching. I’ve basically retrained myself to not have my teeth touch except while eating and talking, but I don’t know if that will cause some new issues down the line. I guess I’ll find out soon enough. And by the way, that tooth was one of those ridiculous sideways growing ones like in your picture!
Aloha Jamie,
Thank you for sharing your story with us! I’m sorry to hear about your pain and discomfort. It sounds like some nerve damage/trauma like we mention in the article, doesn’t it? Bottom jaw, right? This type of impacted, lower jaw wisdom tooth coming in at an odd angle is the most common type to cause nerve trauma.
Keep an eye here as we hope to share a resource that may help folks like you address the stress/challenge to the region.
Aloha!
i have all four of my wisdom teeth both impacted and erupted. I am 38 and my dentist keeps telling me I need to have them removed before they give me problems. he always has a new wisdom tooth horror story for me when I go for my regular cleaning. They used to bother me when they were breaking through the skin but now they are fine. My dad is 62 and he has all four of his as well.
Thank you for sharing your story with us Melissa! Congratulations for not succumbing to the dental horror story strategy. I imagine the dentist is trying to persuade you based on his/her experience with other’s who have problems with their impacted teeth. Because impacted teeth that are not kept clean can cause a bad scene.
Regarding your wisdom teeth, keep ’em clean and you will most likely follow in your wise father’s footsteps!
I had my wisdom teeth removed when I was 25 because I had started forming severe cavitites in them due to me being unable to properly get back there to clean them. However, mine all erupted just fine, with no pain or problems and if it wasn’t for the cavity issues I never would have had them removed. Mine were pulled while I was awake and that also gave me no issues at all. Knowing what I do now, I probably would not have had them pulled and would have tried to find a better way to deal with them since they never gave me any real trouble.
I had very crooked teeth due to having too small of a jaw, and had to have several pulled before getting braces put on. I did have all four wisdom teeth removed, two at a time, as a young adult. One was giving me problems and was infected, but the other three were just done “because they might push my teeth out of alignment in the future”. The first two bottom ones were done in a dentist office with a local anesthetic. I got dry socket in one of them. The top two were done by an oral surgeon and had general anesthesia. I ended up with a perforated sinus and a painful infection.
Aloha Shelley,
Ouch! Sounds like you were one of the statistics when it comes to problems with having wisdom teeth removed! Something about a perforated sinus that makes me shiver. 🙂 In the end, your system was able to get on top of the infection and all is well I presume.
Thank you for sharing your story with us!
I don’t remember how old I was when I had both upper (very long ago and at different times) wisdom teeth removed. They were infected and I do remember having a very swollen face. I did not have any problems with the removal. I still have a lower right wisdom tooth which has not been a problem. My left lower never came in and according to the x-rays does not exist. My mouth is small and I also had 4 molars removed when having braces in my teens to make more room to straighten. I now know that was probably not the best course to take, however, that is what they did at that time. If we only knew then what we know now! Thanks for your article.
Had my wisdom teeth out 35 yrs ago, the flaps/area kept getting infected from food such as sesame seeds, nuts getting trapped/irritated. Don’t think any were sideways. After, my other molars shifted creating a gap where food has jammed increasingly ever since compromising my gum/tooth health. 3 dentists have unsuccessfully tried to build it up. Your applicator & oil has helped +like your floss. Unfortunately the teen you reference has now died. http://bringmethenews.com/2015/06/19/balloons-throughout-eden-prairie-show-support-for-teen-who-died-after-oral-surgery/
Unfortunately the local teen you reference has now died.
Aloha Julie,
Ugg, thanks for letting us know. It seemed that the last we looked, the future wasn’t looking bright for her. Let’s all express a prayer of appreciation for this day and go give a loved one a hug, especially if they aren’t used to receiving one from us recently! I don’t want to even begin to imagine what the parents are going through…
It sounds like you have a mechanical situation that requires regular attention for hygiene similar to a food trap. Knowing that it’s there and having a practiced method to care for it is the game in your case (if I am reading your post right here). We are honored to play a part in helping you with the education and tools necessary to navigate this path to optimal oral health!
Thank you and Aloha!
So far none of my grown children ages 34,23,21&19 have had their wisdom teeth removed & none of them have any complaints to date. According to Weston A Prices research our jaws are smaller since adopting the Standard American Diet.
Agreed on all points Sarah! Thanks for sharing your story with us about your children! Good on you all!
I just took our 5th child age 17 to dentist & her X-ray shows all 4 of her wisdom teeth growing in sideways! Have you all heard of this before?
Good article! My wisdom teeth were described as “impacted” by my dentist when I was 22 years old. But he didn’t push me to get them out if there wasn’t any pain.
I’m 47 years old now. No problems! 🙂
Woot Renee!
Glad to hear that you had a dentist that was willing to leave a tooth alone if it’s healthy!
Thank you and Aloha!
Do you do anything special to keep them clean way back there or just normal care and have been fine?
Have all 4 of my wisdom teeth intact…am 41 with no problems keeping them in…a big Mahalo for this article!
Thanks for the good word Amy! Good on you for such a feat of ‘peaceful resistance’ in this modern age! 🙂 Aloha!
Do you do anything special to keep them clean way back there or just normal care and have been fine?
Thank you so much for this and other informative articles. I am so happy to have access to this type dental information!
Thank you Lyn for your kind words of support. We do appreciate hearing that our work helps you!
I am scheduled to get my wisdom teeth out soon as the 2 top ones are severely decayed and the bottom 2 have cavaties as well. Not thrilled about it, but for me I think it might be the best option. I’m 34, and have way too many cavaties in my mouth currently. Dentist thinks removing these might help with my headaches and not being able to fall asleep at night. I’m really looking for answers as I do not eat a processed diet, take FCLO, etc.
Aloha Danielle,
Thanks for stopping by to share your story with us. We acknowledge you in your decision. Making the best decision isn’t always easy. But since our #1 desire is to support you in greater self empowerment, that you have chosen this is wise. Clearly, the headaches could be related.
Regarding headaches and not falling to sleep easily, you might want to consider removing some common insults to our immune systems. Gluten seems to be the biggest bully in our modern times. Speaking as someone who has dealt with my share of headaches, cutting gluten for me has made a substantial improvement in lowering the headaches (which after all are really just one or another form of response to inflammation). There is lots on this subject, you may want to check out our friend, Sean Croxton, of Underground Wellness for some great resources. Dr Perlmutter recently put out a new book on brain issues and diet. Perhaps my favorite (so far) is ‘Why Isn’t My Brain Working?” by Dr Datis Kharrazian (only if you want to take a deep dive into the issue! 🙂
We hope that helps!
It may be the amount of sugar you are inadvertently cutting out rather than the gluten. I cut sugar out and completely got rid of my chronic headaches and migraines no matter how many of my triggers were set off. Sugar also taxes your immune system, so cutting it will help your teeth in that way, too.
Hi oralWellness, I love your articles. I have two partially impacted wisdom teeth, both on the bottom. It seems that over the years, my right wisdom tooth looks like it has erupted. Could that be possible? I am now 34 years old. When I was around 17-25 I was told that I should get all four out. I refused to get my wisdom teeth out when I was younger because it was so expensive and after asking the doctors what was at risk and how I could prevent the problems, it seemed I could handle the management by spending extra time brushing in the back and flossing. I would rinse wih hydrogen peroxide mixed with water before and after brushing, and use baking soda to brush, and floss twice a day. I was serious about prevention! My friends would laugh at me because I would spend maybe 5min just brushing my teeth. But I didn’t want any more cavities and I wanted my mouth to be healthy. My parents didn’t have money to take me to the dentist twice a year while I was a minor. When I became of age to schedule my own appointments and before I adopted my strict oral health regimen, I was scared that I had so much tartar, and had two fillings! It was so bad, I had to schedule two check-ups within a month of each other to get a cleaning, my teeth were just that tartar filled. I swore things had to change. After I found a natural dental oral health program, I would go back in and the dentists would be surprised at how little work they had to do. I felt proud, and that 5 minutes twice a day was worth the smile!
I have been able to maintain this level of care up until recently, until I became burdened these past two years with taking care of various family members, and my own health practices were neglected. Now I am suffering from an inflamed gum behind the left patially impacted wisdom tooth. I am a naturalist at heart, so as much as possible I want to try natural remedies. I have used oregano oil, melaleuca, peppermint oil, myrrh, lavendar, clove, and cinnamon oil–therapeutic grade, unadulterated, supposedly very high quality essential oils.
I feel the most benefit from Cinnamon oil, but all the others I named have helped soothe the pain instanteously and help support the healing of the redness of gums that a few teeth over from the impacted wisdom tooth have had. I also used winter green essential oil on the bottom of my feet before bed. I am really sad to be experiencing this discomfort and decline of my wisdom teeth. It would be a shame to put all that effort into good care all these years and now have to get them out because of too much stress–but I had to take care of family; I had to help my dad, mom, and family through various hospitals stays and I was the closest one to them. I just hope that I can find healing naturally. It is going on three weeks, and I know that I should be making a dental appoitnment soon, to prevent any further nerve damage–if any is not reversible, but I want to think that there is a way to healing, using natural methods. Please help–anyone who thinks they have a bit of info to offer. Any advice is welcome! Please don’t tell me I will have to get them out. 🙂 Thank you!
Aloha Joy,
Thank you for sharing your story with us. I commend you for both taking such care of your oral health in your 20s as well as your commitment to help family in need.
If I were in your shoes, I would schedule an appointment with a dentist and tell them up front that you simply want their diagnostics and opinion on a course of treatment. It may be something simple. Explain to them that you plan to keep your wisdom teeth even if they recommend to have them removed. Explain to them that you understand the relative risks and benefits of keeping wisdom teeth intact and want their help to address the discomfort you have around that one tooth.
As a side note, you may want to have them do what is called a ‘periodontal depth probe’ to test for gum pocket depths around all your teeth. While using essential oils can help tremendously, if the pocket depth is greater than 4mm, what is required is that we learn strategies how to clean the base of those deeper pockets. You see, putting essential oils at the gum line will help, but won’t address the underlying issue.
Please take a moment to check out our Healthy Mouth System. This product contains the education, tools, and feedback necessary for anyone who is serious about taking care of deeper pockets. My guess is you have a deeper pocket around that wisdom tooth.
I hope that helps! 🙂
Thanks again for sharing your story with us!
I would echo Will and Susan’s advice to you: make an appointment with a good dentist, letting the office know up front that all you want is expert information.
I have done that in 5 offices, with courtesy and real respect for the doctors & staffs, and have received valuable insights from all of them, with no hard feelings anywhere.
Now, I always let the receptionist know right up front that my goal is natural remineralization of my teeth and natural dissolution of tartar, and I ask if the doctor offers guidance toward those goals. In one office both the literature and the receptionist were quite clear that the doctor was totally focused on cosmetics. I did not make an appointment there.
Two of the other dentists (mainly their staffs) have been very informative about the rather dramatic improvements that have occurred in my mouth over the past year of following the Orawellness regimens of Bass brushing with micro-strokes, HealThy Mouth and Shine, swishing/pulling, and gum pocket syringing (what I call GPS). Their insights and careful, professional examinations & reports have given me certainty regarding the value of what I have learned from Will and Susan. This stuff really works.
At the same time, the answers I have thoughtfully received (and paid for) in those offices have decimated what faith I had in the current standard dental education and philosophy. I am grateful for what I continue to learn here.
Thanks for this article! Wish I had known about it earlier, before I had my children get theirs extracted. I had my top wisdom teeth removed when I was 29. I didn’t have any lower wisdom teeth, so didn’t need to worry about them. The extraction went quickly and painlessly, and I was so happy it was such a breeze. That is, until the next day, when I woke up, took a drink, and the water came out my nose! A perforation had occurred that went into my sinus cavity, and I ended up with an extremely painful surgery grafting tissue from my cheek to repair the damage. I was out of work for nearly a week. So far my kids haven’t had any similar problems, although my son’s mouth took longer to heal than my daughter’s. We’ll see over time if there are further implications. Thank you again for all the valuable advice that you post!!!
Aloha Katherine,
Thank you for the kind words of support! I’m sorry to hear that you had your sinus perforated by the extraction process! That’s one of the (many) problems that can occur. We are glad to hear that your kids have been spared any of the funky issues that can occur.
We are honored to be part of your team to help you navigate your path to optimal oral health!
And about the dry socket, I think
there is a solution:Alveogyl to fill The empty
alveolar cavity ,
Then, the two sides of gingiva must
be pressed with your thumb and your finger.
I’m a dentist , and I think that Wisdom teeth must be
removed as soon as they are erupted, around 18 years old ,because their
apex is not copleatly formed by that time so
it has less chance to damage the nerve
And those who are unerupted, in wrong
position … only surgery will solve the problem
Thankyou Orawellnes about the question
Aloha Elona (that sounds nice together! :))
Thank you for sharing your expert feedback here with us. We appreciate and respect your educated opinion on this subject. Like so many subjects, it always amazes me how there can be such disparity of opinions of what is ‘right’ on a given procedure even among the professionals in the field!
So much to learn and study! 🙂
Dr. Elona,
My question to you is, why remove it if it is not bothering you. Don’t you think instead of promoting removal dentist should be looking for a way of cleaning the wisdom teeth since they are “far behind” and difficult to clean?
I’m 38 years old and I still have 2 wisdom teeth. Only one of them has protruded past the gum line and the other tooth has not moved. Neither tooth causes me ANY pain or discomfort. Why would I spend money and go under anesthesia if I do not have to? If my appendix isn’t causing me any problems should I gave that removed too? Which brings me to something my mother used to tell me when I told her that “it hurts when I do this___!” She would reply, “Well then DON’T do [THAT]!” If it aint broke don’t fix it! If my wisdom teeth aren’t causing any problems whatsoever, then leave them alone I say.
I’ve had dentists telling me to remove my wisdom teeth since I was I. High school. They told me they they were at risk of decay, hard to clean, and would crowd my teeth out. I’m now 45 with all my wisdom teeth, they finished coming out of my gums in my 40s. They require a little extra cleaning, but everything I was told never came to be. I’m glad You didn’t listen to my dentists. I actually don’t trust them either. I had some teeth reminineralize and heal from the cavities on their own. My dentist told me that this occasionally happens. Really? Then why isn’t this info more widely know or understood?
How can it be “right” to indiscriminately remove everyone’s wisdom teeth at 18 years old? People are individual, and removing one person’s teeth at all can damage their nervous system and bite. In my case, with a high angle bite and long face, wisdom teeth created a massive shift that ultimately destroyed my ability to play piano with the same agility. it’s scary to see doctors think that they should just go about removing people’s organs, and teeth are organs, they even sit on important acupuncture meridian lines. I know that you will feel threatened by this and think that you deserve to be making 10’s of thousands a year off pulling out people’s teeth, but you don’t. You swore to first do no harm. Dentists can cause so much harm, and orthodontists, too. Invisalign, all those things, you’re playing with people’s delicate balance and mouth posture, which can lead to facial scoliosis and scoliosis down the back.. There’s a reason dentists have the highest salaries and commit suicide the most. They harm people for profit, all the time.